
People are the most hopeful of the Lymphedema Treatment Act, whose most current bill has already been presented. However, there are some hopeful changes brought in the Medicare coverage system. With all these denials, the process itself becomes an emotional burden on the patient and the financial mountain keeps rising. 
Many cases are denied just because of some laughable reasons like the code are incorrect or the signature does not exactly match etc. Also, undergoing all these procedures involves money and it can become a financial burden too. To obtain any kind of coverage for lymphedema, the patient has to carry a huge data of proof, which becomes a mental burden. As a result, precious time is lost doing all this and the lymphedema progresses to later stages, making it all the more difficult to treat and reverse.Īnother difficulty encountered by lymphedema patients is that lymphedema is classified as a functional disease, whereas in reality it is an illness. When it comes to the supply of some other things, like pumps for the pneumonic compression therapy, one has to first try the basic models of pumps for weeks and weeks and give evidences for its failure, before they can apply for the advanced versions and it gets approved. Some companies do not even agree for services of a specialist they insist that the bandaging process can be done by any trained medical professional. As a result, the chances of infections are much higher, if the proper equipment and treatment is not provided to those affected. Many other private insurance companies also do not include this in their coverage norms. 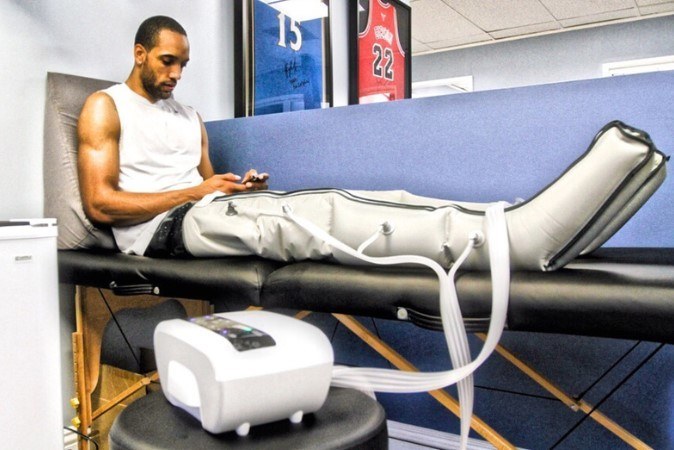
These do not fit properly into any of the categories included in the coverage. Talk with your physical therapist to see what they would recommend for you for your long-term care.The main area of problem in lymphedema insurance approval is the compression garments and supplies. Cold compression therapy certainly aids in the recovery and healing process post-injury, but clients see benefits in daily use as well. 
Some clients decide they want to buy the equipment at the end of treatment or during treatment because they see the benefits to having cold compression therapy to help during all their training and athletic endeavors. VIEW OUR RENTAL PRODUCTS Purchasing Equipment: Many people will rent the equipment to enable them to continue the therapy at home, returning the equipment once healing is complete. Renting the equipment is a viable option that will lower your out-of-pocket expenses considerably. If a doctor instructs you to have cold compression therapy, you need to find a solution if insurance does not cover the prescription. Here are some steps to take if your insurance doesn’t cover this important therapy option: Equipment Rental: Therapies like cold compression systems – for use during and after physical therapy sessions – are gaining acceptance among insurance carriers, especially on Workers’ Comp claims, however, there is still a long way to go until it is covered by most people’s insurance. And, this includes covering devices needed in therapy either during or after client sessions are concluded. The short answer is insurance companies often do not cover this often medically-mandated therapy. (Or worse, they refuse treatment out of fear they will be buried with out-of-pocket expenses when something isn’t covered.) It’s no wonder patients are often left scratching their heads wondering if a doctor-prescribed treatment plan will be covered. So is your cold compression therapy covered? Short answer- it’s complicated. And in addition, understanding what is and isn’t covered on a person’s unique plan is about as easy as understanding the changes in the tax code year in and year out. Every plan is unique to the person or family it covers. Insurance companies, and what they cover, are just about as varied as the stars in the sky or the sand on a beach.
0 Comments
Leave a Reply.AuthorWrite something about yourself. No need to be fancy, just an overview. ArchivesCategories |
 RSS Feed
RSS Feed
